The patient

Patient right profile
Bilateral Asymmetric Keratoconus induced by eye rubbing
Identity : Ms B.T
First visit : 03/28/2017
Last Visit : 06/27/2017
Ms. B.T is a 27-year-old female with no previous medical history or any known keratoconus in her family .
Her refraction at the first visit (03/28th/2017) was: Right eye (RE) 20/32 with -1.5 (-1.75 x 60 °) and Left Eye (LE) 20/40 with -2.25 (-2.75 x 125 °).
Clinical examination with the slit lamp suggested an paracentral irregular inferior corneal thinning and bulge, more pronounced in the left eye .
Corneal topography performed at our institution showed the presence of bilateral keratoconus, more pronounced in the left eye.
She had come to us for a second opinion. The first ophthalmologist that she consulted over several visits had proposed corneal collagen cross-linking, as he had noticed progression in the left eye. The patient showed us a copy of the difference map that she had done previously. Our interpretation of the map was that it showed irregular and random changes but no real progression.
During the first visit, we asked the patient about the possibility of frequent eye rubbing. She claimed that she was not really aware of such a habit. When we examined her fingers, we noticed that they were stained with eye make-up (mascara / eye liner). We suggested to the patient to become aware of the possibility that she was rubbing and touching her eyes unconsciously and more often than she realised.
At her second visit, the patient acknowledged that she was rubbing her eyes quite often during the day. While working on the computer, she would sometimes press her palms against her orbits and perform circular movements. She verbalised that since her vision had deteriorated, she was even more inclined to touch her eyes.
We explained to the patient that she was rubbing her eyes excessively, and explained the mechanism of cornea deformation in keratoconus to be repetitive local trauma. While she promised to pay attention to this, she warned us that it would be quite difficult for her to stop eye rubbing, as it had become a pleasurable and « useful » habit. Eventually, she promised to do everything to stop this bad habit, and we provided her with another appointment three months later.
Here are pictures of the patient rubbing her eyes and her profiles
 PATIENT RIGHT PROFILE
PATIENT RIGHT PROFILE PATIENT LEFT PROFILE
PATIENT LEFT PROFILE PATIENT SHOWING HER SLEEP POSITION (LEFT SIDE). This position may favor chronic irritation and contamination of the left eye, leading to more itch and eye rubbing.
PATIENT SHOWING HER SLEEP POSITION (LEFT SIDE). This position may favor chronic irritation and contamination of the left eye, leading to more itch and eye rubbing. PATIENT SHOWING HOW SHE RUBS HER EYES (USING FISTS)
PATIENT SHOWING HOW SHE RUBS HER EYES (USING FISTS) PATIENT RUBBING HER EYES (WITH FINGERS AND NAILS)
PATIENT RUBBING HER EYES (WITH FINGERS AND NAILS) PATIENT'S EYES AFTER UNCONSCIOUS RUBBING (NOTE THE SMEARED MASCARA)
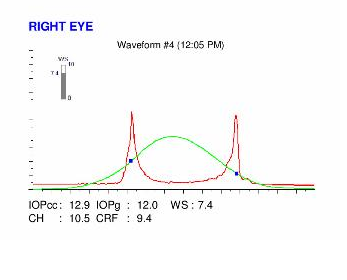
PATIENT'S EYES AFTER UNCONSCIOUS RUBBING (NOTE THE SMEARED MASCARA)Here are the Orbscan quadmaps, Pentacam maps, OPDscan (topography and aberrometry) maps and Ocular Response Analyzer (ORA) results of the first visit .
Difference maps were performed at each subsequent visit. At the second visit, the patient confessed to having a habit of pressing her orbits vigorously with her palms many times a day. She had not realized till then that this constituted a form of repetitive trauma to the eyes. She had also tried to modify her sleeping position to avoid extended compression of her left orbit.
 PATIENT SHOWING HOW SHE PRESSES HER ORBIT WITH HER PALMS
PATIENT SHOWING HOW SHE PRESSES HER ORBIT WITH HER PALMSNo evolution has been observed between the first and last visits. The keratoconus is stable, more than 3 months after the patient definitively stopped rubbing her eyes . CXL (cross linking) was not necessary to attain stabilisation in her case, but the cessation of eye rubbing was. This case is an eloquent demonstration that eye rubbing is often an unconscious habit of some patients. It is important to take time to investigate and elucidate the possibility of unconscious eye rubbing in patients, and to eradicate all gestures and postures that could be detrimental to corneal stability.
In this case, the frequency and intensity of eye rubbing developed progressively. Eye rubbing provided pleasurable and relaxing sensations, but progressively caused the cornea to deform and the vision to degrade. This degradation of vision evoked a eye rubbing response in the patient, and the vicious circle ensued. She did not acknowledge chronic eye rubbing at the first visit, although there existed some indirect evidences of her habit. At the second visit, the patient confessed to rubbing her eyes repeatedly and vigorously, sometimes with the palms of her hands, just to « relax even more » when tired at the computer. Abandoning eye rubbing was difficult but rewarding in the end, as no progression has been observed since.