Patient right profile
Case #71
The patient

Unilateral Asymmetric Keratoconus induced by eye rubbing
Identity : Mr C.T
First visit : 09/05/2017
Last Visit : 01/23/2018
Mr. C.T is a 30-year-old male car mechanic with no previous medical history or any known family history of keratoconus. He has no history of atopy. He presented to us with a progressive decrease in visual acuity greater in the right eye than the left.
He was diagnosed with keratoconus in another institution, where he was followed for 2 years. As the keratoconus in his right eye was progressing, he was referred to us for a second opinion and management.
His refraction at the first visit at the Rothschild Foundation (on 09/05th/2017) was : Right Eye (RE) 20/32 with+0.25 (-2.5 x 70 °) and Left Eye (LE) 20/20 with -0.5 (-0.75 x 115 °).
Clinical examination with the slit lamp suggested a thin and irregular right cornea with a Fleischer ring. Fleischer rings are pigmented rings in the peripheral cornea, resulting from iron deposition in basal epithelial cells, in the form of hemosiderin.
Corneal topography performed at our institution showed the presence of bilateral keratoconus, more pronounced in the right eye.
At the first visit, when asked about the possibility of frequent eye rubbing, the patient admitted to rubbing his eyes when he awoke in the mornings or at work because of the hot temperature of the garage which made him sweat a lot.
He is right-handed and admitted to rubbing his right eye more than the left. He would use the back of his right hand and forearm to wipe the sweat from his brow while at work, and would simultaneously rub his right eye with the upper arm or forearm. He avoided using his fingers to rub the eyes since he considers them dirty from the engine and gear dust or oil acquired at work. The patient sleeps on his right side with the head buried in the pillow (pillow hugging).
At the subsequent visits, after having benefited from the information he received at the first visit, he admitted to realizing that he was rubbing his eyes more than he had thought, not only during his work shifts but also in the mornings upon awakening.
We explained to the patient that since vigorous rubbing had preceded the drop in visual acuity, this habit may have caused the cornea to deform, leading to the classic clinical presentation of keratoconus in his case.
We strongly advised this patient to stop rubbing his eyes and to change his unhealthy sleeping position. We prescribed him eye shield protection for sleep and at work.
He subsequently stopped rubbing his eyes at work and altered his sleeping position.
Here are pictures of the patient rubbing his eyes and his profiles
 PATIENT RIGHT EYE PROFILE
PATIENT RIGHT EYE PROFILE PATIENT LEFT EYE PROFILE. The upper and lower eyelids were retracted by the examiner.
PATIENT LEFT EYE PROFILE. The upper and lower eyelids were retracted by the examiner.  PATIENT RUBBING HIS EYE WITH THE BACK OF HIS HAND AND HIS FOREARM
PATIENT RUBBING HIS EYE WITH THE BACK OF HIS HAND AND HIS FOREARM PATIENT DEMONSTRATING HIS SLEEPING POSITION. The patient sleeps on the right side and applies his head against his arm. While doing this, the right orbital area is in direct contact with the arm.
PATIENT DEMONSTRATING HIS SLEEPING POSITION. The patient sleeps on the right side and applies his head against his arm. While doing this, the right orbital area is in direct contact with the arm.Here is a video of the patient demonstrating how he rubs his right eye with his upper arm while at work.
EXAMINATIONS PERFORMED IN ANOTHER INSTUTION
Here are the patient’s examinations performed in another institution in France between 2014 to 2016, before his first visit to the Rothschild Foundation in Paris. The topographies show progression of the keratoconus in the right eye.
EXAMINATIONS PERFORMED IN FRANCE – ROTHSCHILD FOUNDATION – PARIS
Here are the Orbscan quadmaps, Pentacams maps, OPD scans and Ocular Response Analyzer (ORA) results of the first visit at our institution.
 RIGHT EYE ORBSCAN (1st VISIT). Note the increased prolateness (negative asphericity) and toricity (astigmatism) of the anterior (top right) and posterior (top left) corneal surfaces (island pattern). On the curvature map (bottom left), irregular astigmatism is characterized by a marked inferior and temporal steepening. The thickness map (bottom right) shows central thinning with slight displacement of the thinnest point.
RIGHT EYE ORBSCAN (1st VISIT). Note the increased prolateness (negative asphericity) and toricity (astigmatism) of the anterior (top right) and posterior (top left) corneal surfaces (island pattern). On the curvature map (bottom left), irregular astigmatism is characterized by a marked inferior and temporal steepening. The thickness map (bottom right) shows central thinning with slight displacement of the thinnest point.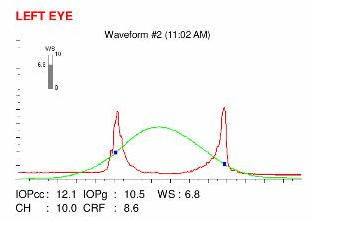 LEFT EYE ORA (Ocular Response Analyzer). The ORA measurement of the left eye is unremarkable, despite a slight reduction in the height of the peaks. The left eye is not rubbed as often and as vigorously as the right eye, explaining the preservation of the corneal biomechanical properties explored by this instrument.
LEFT EYE ORA (Ocular Response Analyzer). The ORA measurement of the left eye is unremarkable, despite a slight reduction in the height of the peaks. The left eye is not rubbed as often and as vigorously as the right eye, explaining the preservation of the corneal biomechanical properties explored by this instrument.Difference maps were performed at each subsequent visit. No evolution was observed between the first and last visits. The keratoconus is stable, more than 4 months after the patient definitively stopped rubbing his eyes .
This is an intriguing and informative case that highlights the causal effect of eye rubbing on the genesis of keratoconus. The asymmetry in the corneal deformation between right and left eyes resides in the fact that the patient predominantly rubbed his right eye. Like many of the other cases described in this site, the eye rubbing habits are determined by the patients’ occupations (computer analyst using the mouse, mechanic, engineer etc). In this case, the right-handed car mechanic uses his right arm and the back of the hand to wipe sweat off his brow and simultaneously rubs his right eye. This patient also sleeps on the right side, and it is possible that chronic ocular compression by the pillow and contamination from the linen irritates the right eye further, causing pruritus. Rubbing results in temporary relief, but aggravates the situation by adding more germs and irritants to the ocular surface. It then triggers more rubbing, causing the cornea to deform progressively.
Most medical text books would attribute keratoconus to unknown genetic factors. Genetics alone would not explain the unilateral occurrence of keratoconus in many cases, while eye rubbing does very well (unilateral rubbing causes unilateral keratoconus). Genetics however, may account for increased ocular sensitivity, atopy, and reduced corneal resistance to repeated trauma.
The cessation of rubbing in this case has arrested the progression of keratoconus.
Autres cas :
- Date 28 janvier 2018
- Tags Enjoyed eye rubbing, Eye rubbing, Forme frustre keratoconus (FFKC), Inferior keratoconus, Knuckles rubbing, Male, Morning rubbing, Sleep position, Unilateral keratoconus, Work rubbing






















